Simulation is not just about technology; it is about changing the way we think about education and patient safety.
— Willem van Meurs, 2024
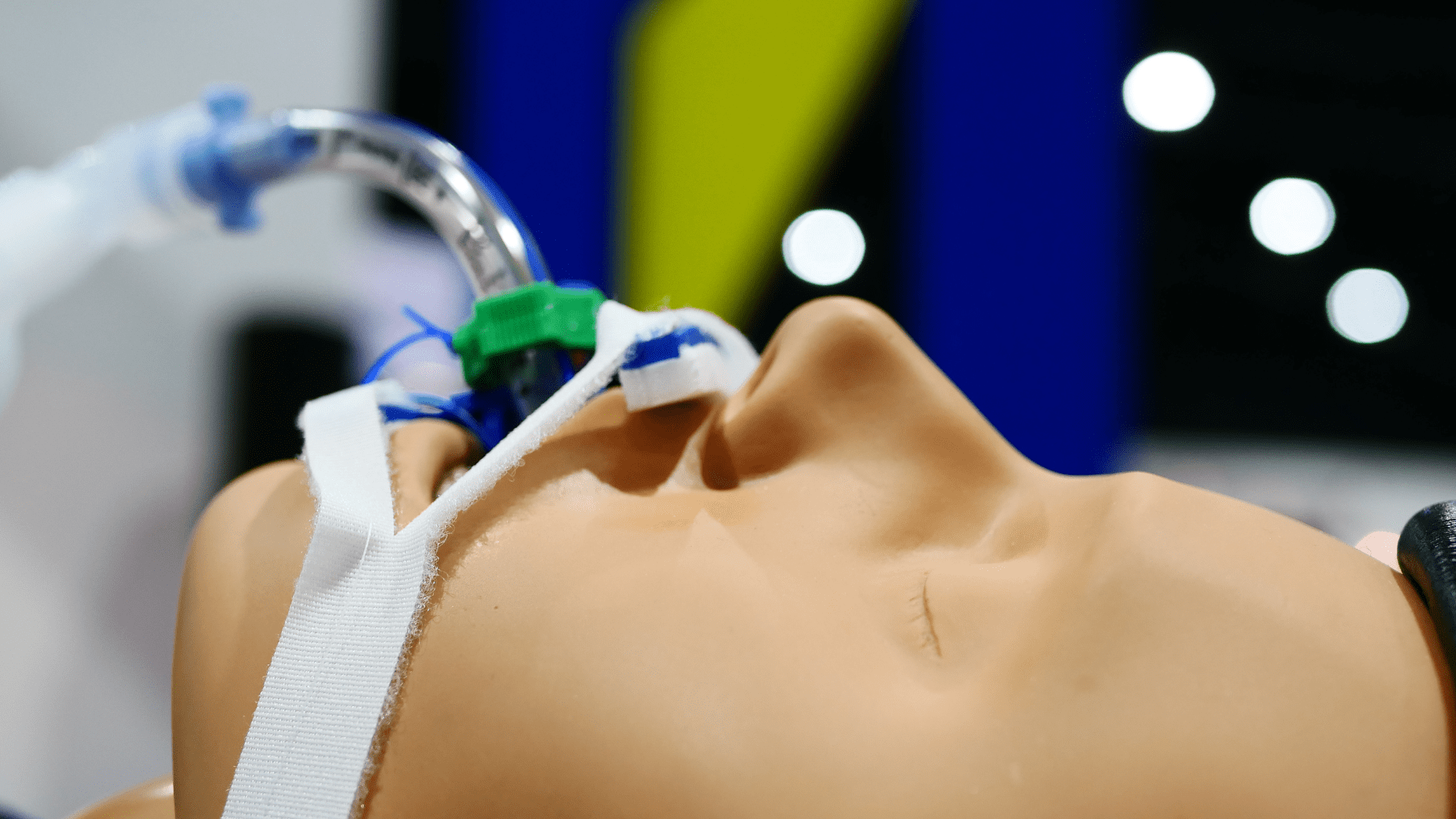
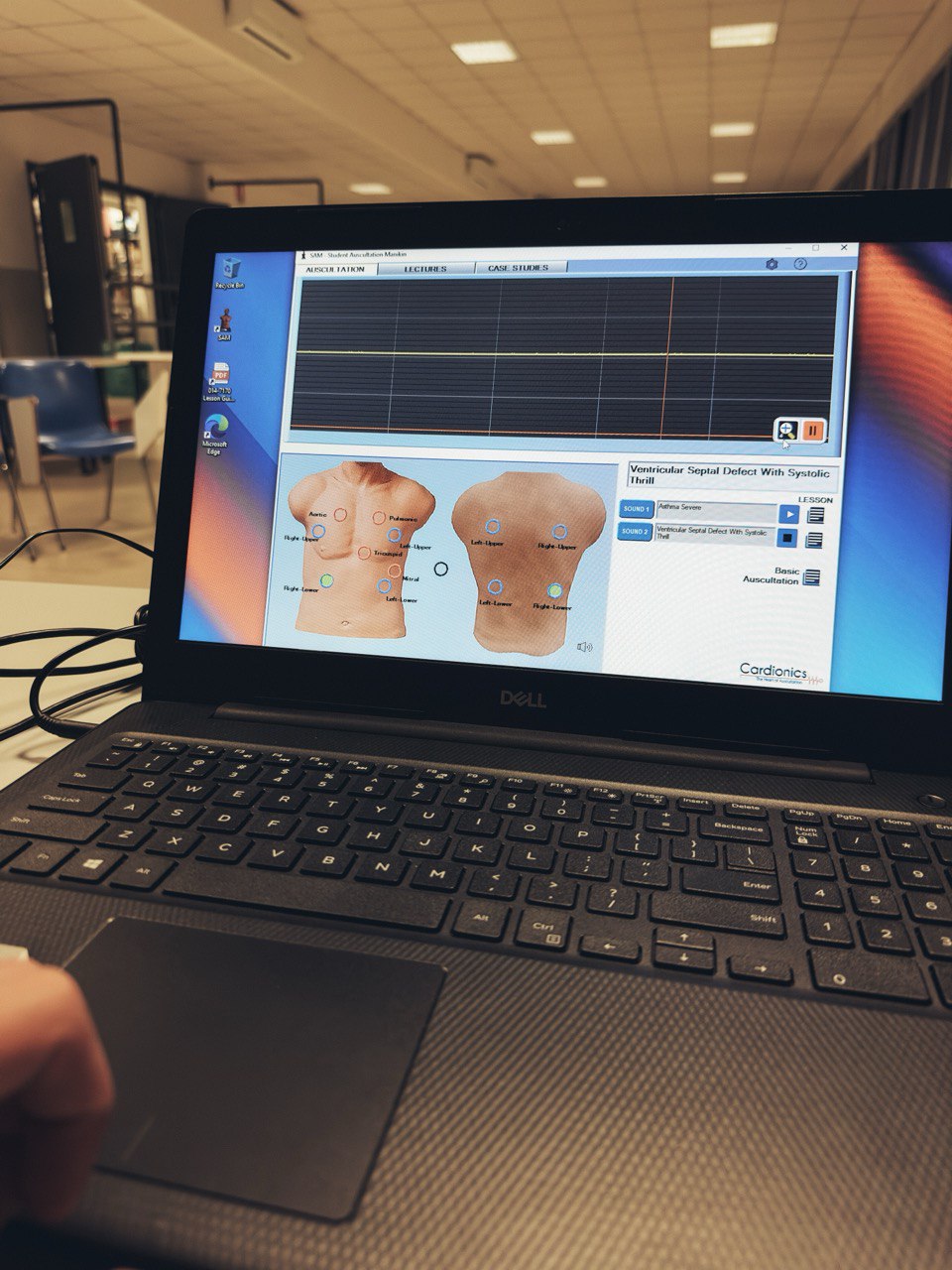
Medical simulation has evolved from simple mannequin-based training to complex virtual reality environments that can replicate critical clinical scenarios with unprecedented fidelity and realism.
Briefing
Prepare participants with objectives, roles, and clinical context before the simulation begins.
Simulation
Run the scenario with real-time monitoring, allowing learners to apply clinical reasoning and teamwork.
Debriefing
Facilitate reflective discussion to consolidate learning and identify areas for improvement.
Key Finding: Studies show that simulation-based medical education improves clinical outcomes by 25-40% compared to traditional didactic methods, with the greatest improvements observed in procedural skills and team communication.
| Feature | Low Fidelity | High Fidelity |
|---|---|---|
| Realism | Basic task trainers, partial models | Full-body mannequins with physiological responses |
| Cost | $500 – $5,000 | $50,000 – $250,000 |
| Best For | Skill acquisition, basic procedures | Team training, crisis management |
| Setup Time | Minutes | Hours |

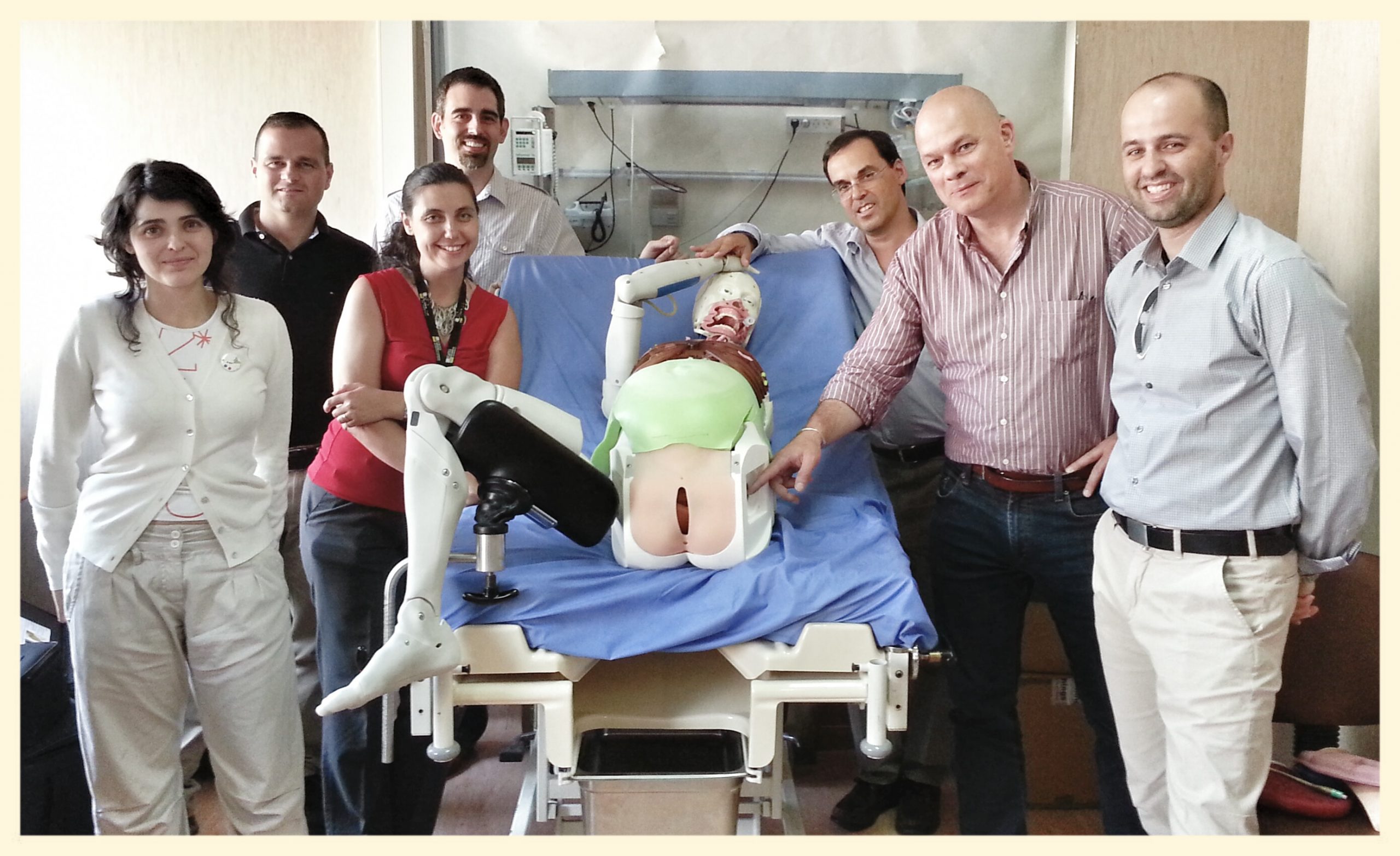
The SIMZINE team at EuroMedSim 2024, Stuttgart
Pre-Simulation
Orientation to equipment, environment familiarization, and review of learning objectives with all participants.
Active Simulation
Real-time clinical scenario with patient deterioration, requiring team-based decision making and intervention.
Post-Simulation
Structured debriefing using advocacy-inquiry method, video review, and action planning for clinical practice.

Fig. 1 — State-of-the-art simulation center at EuroMedSim



- Establish clear learning objectives aligned with clinical competencies and patient safety goals.
- Select appropriate simulation modality based on educational needs and available resources.
- Train facilitators in both technical operation and educational debriefing methodologies.
- Implement structured assessment tools to measure learning outcomes and program effectiveness.
- Create a culture of psychological safety that encourages open discussion and reflective practice.
| 1 | Needs Assessment: Identify the clinical competencies and skills gaps that simulation training should address. |
| 2 | Curriculum Design: Develop structured learning pathways with progressive complexity and clear milestones. |
| 3 | Resource Allocation: Secure funding, equipment, space, and trained personnel for sustainable program delivery. |
| 4 | Quality Assurance: Monitor outcomes, collect feedback, and continuously refine scenarios and teaching methods. |
1. McGaghie WC, et al. A critical review of simulation-based medical education research. Medical Education. 2010;44(1):50-63.
2. Issenberg SB, et al. Features and uses of high-fidelity medical simulations. Academic Medicine. 2005;80(10):957-967.
3. Cook DA, et al. Technology-enhanced simulation for health professions education. JAMA. 2011;306(9):978-988.